
Located in the Darya Ganj, Neera Eye Centre believes that clear vision is essential for a good quality of life.
As a top eye care facility, we use the latest technology and show lots of care to help you see the world more clearly.
Dr. Neera Aggarwal passed her MBBS and MS from King George Medical College, Lucknow in 1991. She was a Senior Resident Surgeon at the same hospital for one year.
With over 30 years of experience, Dr. Neera has performed thousands of Lasik surgeries, cataract procedures, and cornea transplants. She was a senior consultant at Max Hospital and has been a guest speaker at many National and International conferences.
We offer a wide range of eye care services, from routine checkups to advanced surgical treatments, all under one roof.
We specialize in advanced treatments including Cataract Surgery, LASIK, Corneal Transplants, and Retina Services.
Our team ensures you feel comfortable, understood, and cared for every step of your treatment journey.




Delhi, the capital of India, has a rich history. The city is dotted with spellbinding mosques, forts, and monuments left over from the Mughal rulers that once occupied the city. The contrast between rambling Old Delhi and well planned New Delhi is immense, and it's interesting to spend time exploring both. If you feel in need of some relaxation, just head to one of Delhi's flourishing landscaped gardens. Here's a list of the top 10 Delhi attractions.
Read More
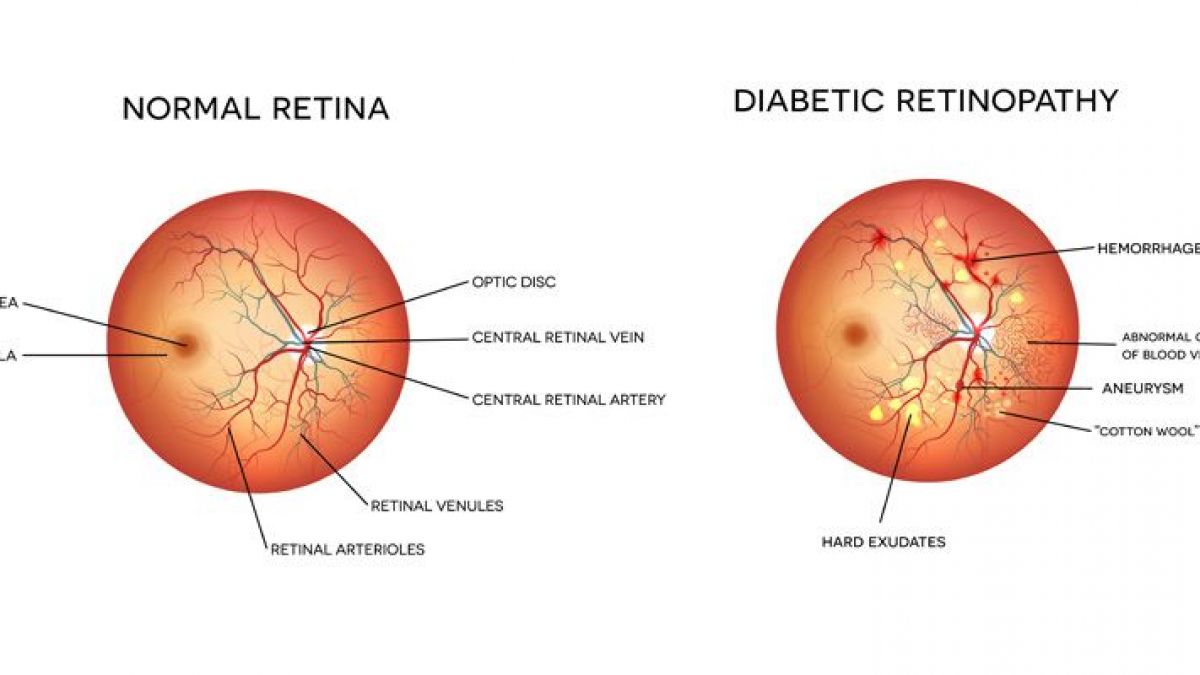
Diabetic Retinopathy: The Silent Vision Killer You Shouldn’t Ignore

Contact Lens Hygiene

Protect Your Eyes: Top 7 Everyday Habits to Prevent Eye Injuries